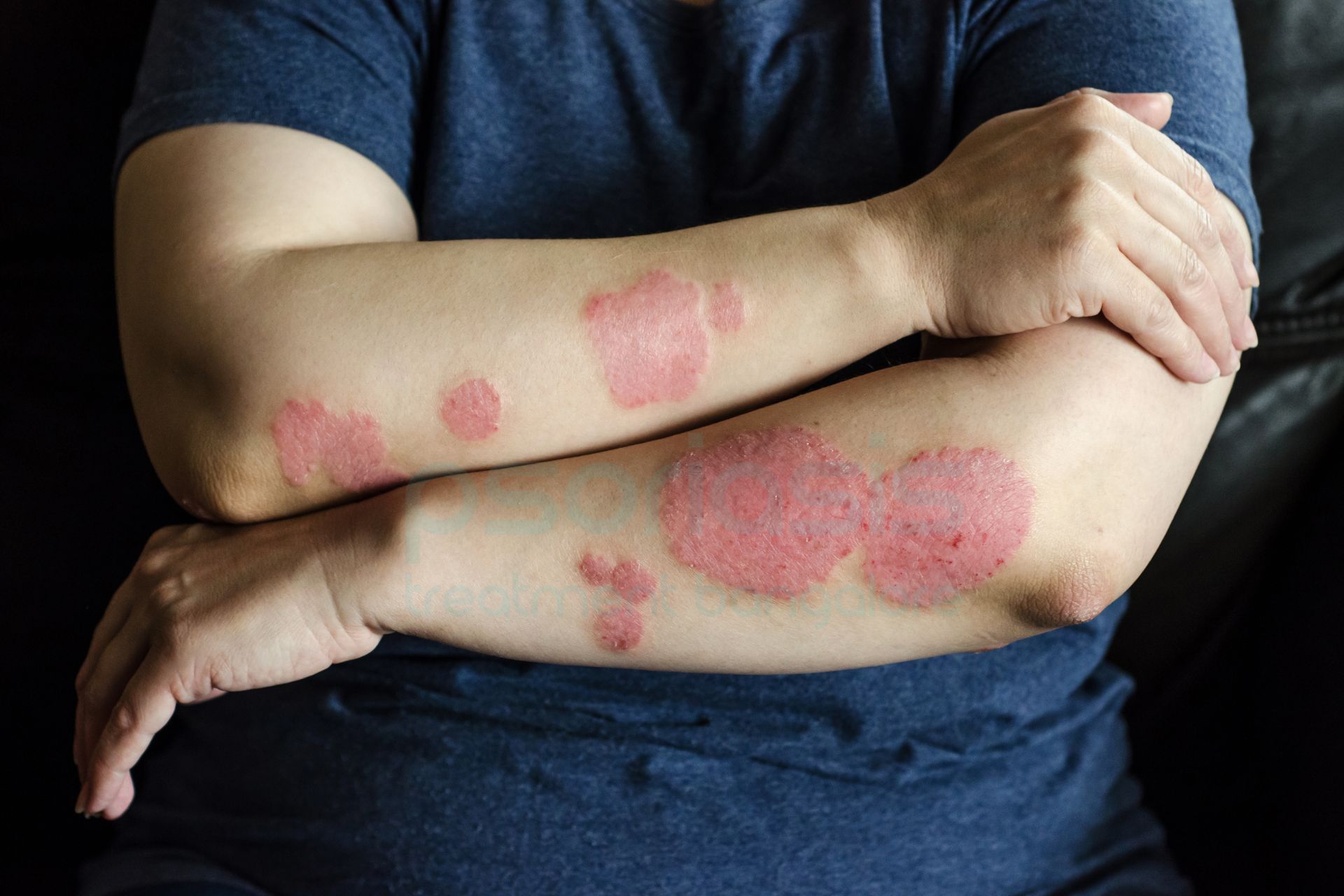
A Comprehensive Guide to Understanding Psoriasis and Ayurvedic Management
Skin diseases are among the most visible health conditions individuals can experience. While many skin issues resolve spontaneously, others persist as chronic challenges that continue to perplex modern medicine—not only due to their enduring nature but also because of their significant impact on physical appearance and psychological well-being.
Unlike conditions such as diabetes or hypertension, dermatological disorders are immediately visible, affecting self-perception, confidence, and social interaction. These visible changes can lead to emotional distress, diminished self-esteem, social isolation, anxiety, and depression.
Among these challenging conditions, psoriasis remains particularly significant.
The Psychological Burden of Skin Diseases
To appreciate the emotional impact of psoriasis, consider the common experience of acne. Many recall the distress of adolescent acne: constant self-monitoring, experimental treatments, and the discomfort of visible skin changes.
Now consider a condition that:
- Persists chronically rather than resolving quickly
- Features recurring flare-ups
- Affects visible body areas
- Requires lifelong management
This represents the daily reality for individuals living with psoriasis.
Defining Psoriasis
The term “psoriasis” derives from Greek etymology: “psora” (itch) combined with “iasis” (condition), literally translating to “an itching condition.”
Medically, psoriasis is classified as a systemic, immune-mediated inflammatory disorder primarily affecting the skin and occasionally the joints. It represents an autoimmune condition where the immune system erroneously targets the body’s own tissues, resulting in accelerated skin cell turnover and chronic inflammation.
Psoriasis as an Autoimmune Disease
Autoimmune diseases occur when the immune system reacts against the body’s own tissues. These conditions may be systemic (affecting multiple organs, such as lupus) or organ-specific (targeting a single tissue type, such as thyroiditis).
Psoriasis belongs to the category of immune-mediated inflammatory skin diseases, with potential joint involvement in certain cases.
Clinical Presentation
Psoriasis typically manifests as:
- Red or salmon-pink elevated patches
- Silvery-white scales
- Dryness and fissuring
- Pruritus or burning sensations
- Nail changes, including pitting
Disease severity varies considerably between individuals, with symptoms fluctuating over time.
Common Clinical Features
- Silvery-white scaling
- Erythematous, raised plaques
- Persistent pruritus
- Nail pitting or discoloration
- Lichenified skin patches
- Joint stiffness in select cases
Etiology of Psoriasis
Despite recognition as a distinct disease entity since Willan’s 1808 classification, the precise etiology of psoriasis remains incompletely understood. Research indicates a multifactorial pathogenesis involving complex interactions between numerous elements.
Contributing Factors
- Genetic predisposition
- Immune system dysregulation
- Physical trauma (Koebner phenomenon)
- Infectious triggers
- Certain medications
- Ultraviolet light exposure
- Metabolic factors
- Hormonal fluctuations (pregnancy, menopause)
- Alcohol consumption and tobacco use
- Chronic psychological stress
- Obesity
This multifactorial nature explains the considerable individual variation in disease presentation and progression.
Classification of Psoriasis
Psoriasis can be classified by morphological type, anatomical distribution, and disease severity.
Morphological Classification
Plaque Psoriasis (Psoriasis Vulgaris)
The most prevalent form comprises approximately 80% of cases. Characterized by erythematous, elevated plaques with silvery-white scales. Common anatomical sites include the scalp, elbows, knees, umbilical region, and buttocks.
Guttate Psoriasis
Presents with small, droplet-shaped erythematous lesions, typically on the trunk. Affects approximately 2% of psoriasis patients and often follows streptococcal infections.
Linear Psoriasis
A rare variant following Blaschko’s lines.
Follicular Psoriasis
An uncommon form, with higher prevalence in pediatric populations.
Pustular Psoriasis
Characterized by sterile pustules with surrounding erythema and scaling. May occur independently or alongside plaque psoriasis.
Erythrodermic Psoriasis
A severe inflammatory variant involving widespread erythema and scaling across the majority of body surface area. Often evolves from unstable plaque psoriasis.
Unstable Psoriasis
Acute exacerbation of previously stable chronic disease.
Anatomical Classification
Scalp Psoriasis
Affects approximately 50% of psoriasis patients and frequently represents the initial site of involvement. Symptoms include pruritus, desquamation, and potential alopecia. Distinguished from seborrheic dermatitis by plaque extension beyond the hairline and characteristic silvery-white scaling.
Inverse (Flexural) Psoriasis
Occurs in intertriginous areas, including axillae, groin, inframammary regions, and gluteal folds. Lesions appear smooth and inflamed with minimal scaling due to moisture retention.
Palmoplantar Psoriasis
Affects palms and soles, causing hyperkeratosis, scaling, and painful fissures. More prevalent in women and frequently impairs functional activities.
Nail Psoriasis
Present in up to 40% of patients, particularly those with psoriatic arthritis. Clinical signs include nail pitting, oil drop sign, onycholysis, and discoloration.
Genital Psoriasis
Occurs in 30–40% of patients across all age groups. Often presents as inverse psoriasis with smooth erythematous lesions.
Mucosal Psoriasis
Includes geographic tongue and fissured tongue, commonly associated with pustular variants.
Ocular Psoriasis
Affects approximately 10% of patients, with male predominance. Manifestations include blepharitis, conjunctival xerosis, and uveitis. Untreated cases may result in visual complications.
Severity Classification
- Latent Psoriasis: Minimal lesions, subtle symptoms resembling dandruff, nail pitting
- Mild Psoriasis: Body surface area (BSA) involvement <10%
- Moderate Psoriasis: BSA involvement >10%
- Moderate to Severe: Significant functional and psychosocial impairment
- Severe Psoriasis: BSA >20%, unstable lesions, increased arthritis risk
Associated Complications
Clinical studies demonstrate potential associations between psoriasis and:
- Severe pruritus
- Eczematization of lesions
- Secondary bacterial infections
- Psoriatic arthritis
- Psychological comorbidities
- Metabolic syndrome and systemic complications
Diagnostic Evaluation
Diagnosis is predominantly clinical, based on characteristic morphological features. When clinical presentation is atypical, investigations may include:
- Skin biopsy with histopathological examination
- Complete blood count (CBC), erythrocyte sedimentation rate (ESR)
- Lipid profile
- Hepatic and renal function tests
- Rheumatoid factor, antinuclear antibody (ANA)
- Urinalysis
These investigations assess disease activity, exclude infectious etiologies, and evaluate systemic complications.
Conventional Treatment Approaches
Psoriasis management remains clinically challenging. Therapeutic selection depends on patient age, disease severity, and progression patterns.
Standard approaches include:
- Symptomatic management of pruritus and discomfort
- Topical pharmacotherapy
- Phototherapy (UVB, PUVA)
- Systemic medications
- Biologic agents
Each modality presents distinct benefits and limitations, requiring individualized treatment planning.
Psychosocial Impact
Psoriasis significantly affects emotional well-being. Many individuals experience:
- Diminished self-esteem
- Social embarrassment and isolation
- Anxiety and depressive symptoms
- Reduced occupational productivity
- Interpersonal relationship challenges
Addressing psychological health is equally important as treating physical manifestations.
Ayurvedic Understanding of Psoriasis
In Ayurveda, psoriasis is classified under Kushta, a group of dermatological disorders arising from dosha imbalance. This imbalance primarily results from:
- Improper dietary patterns
- Irregular lifestyle practices
- Compromised digestive function
- Psychological stress
Ayurveda conceptualizes psoriasis as a systemic condition rather than an isolated dermatological disorder.
Ayurvedic Treatment Framework
Ayurvedic management emphasizes root-cause correction rather than symptomatic suppression.
Two-Phase Treatment Protocol
1. Purificatory Treatment (Shodhana/Panchakarma)
Indicated when doshas are significantly aggravated and appropriate for elimination. Patient eligibility requires careful assessment.
2. Palliative Treatment (Shamana)
Comprises internal Ayurvedic formulations and external applications. The majority of psoriasis patients respond favorably to this phase.
Dietary and Lifestyle Modifications
Diet and lifestyle represent central pillars of Ayurvedic care. Without addressing these factors, treatment outcomes may be suboptimal.
Common Dietary Recommendations
Minimize or avoid:
- Excessive sour, salty, and pungent foods
- Frequent curd and incompatible milk combinations
- Jaggery and sesame products
- Black gram preparations
- Alcohol and tobacco
Treatment Duration
Response to Ayurvedic treatment varies based on:
- Disease severity and chronicity
- Adherence to dietary and lifestyle modifications
- Individual constitutional factors
The therapeutic goal emphasizes gradual, sustained improvement rather than immediate symptom suppression.
Ayurvedic Psoriasis Treatment in Bangalore
Total Ayurveda offers comprehensive Ayurvedic psoriasis treatment in Bangalore, distinguished by:
- Over a decade of clinical experience
- Evidence-based, ethical Ayurvedic practice
- Personalized treatment protocols
- Traditional herbal oil-based dermatological support
Conclusion
Psoriasis affects approximately 2–3% of the global population. This chronic, recurrent condition can profoundly impact quality of life. While an immediate cure may not be achievable, consistent, informed, and holistic management can produce meaningful clinical and psychosocial benefits.
If you are living with psoriasis, comprehensive support is available.
Schedule a consultation with Total Ayurveda to explore personalized Ayurvedic treatment options.
PS: This information is educational and not a substitute for professional medical advice. Always consult qualified healthcare providers for diagnosis and treatment decisions.
Frequently asked questions
1. What exactly is psoriasis?
Psoriasis is a chronic, immune-mediated inflammatory skin condition that causes red, scaly patches, itching, and recurring flare-ups. It is not contagious.
2. Is psoriasis an autoimmune disease?
Psoriasis is classified as an immune-mediated inflammatory condition where the immune system triggers excessive skin cell growth and inflammation.
3. What are the early signs of psoriasis?
Early signs may include persistent dandruff-like scaling, red patches on the skin, itching, nail pitting, or dry, flaky areas that do not heal easily.
4. What causes psoriasis flare-ups?
Flare-ups can be triggered by stress, infections, skin injury, certain medications, alcohol, smoking, hormonal changes, and lifestyle factors.
5. What are the different types of psoriasis?
Common types include plaque psoriasis, scalp psoriasis, guttate psoriasis, pustular psoriasis, inverse psoriasis, palmoplantar psoriasis, and erythrodermic psoriasis.
6. Can psoriasis affect areas other than the skin?
Yes. Psoriasis can affect nails, joints (psoriatic arthritis), scalp, eyes, and mucosal areas in some individuals.
7. How is psoriasis diagnosed?
Psoriasis is usually diagnosed through clinical examination. In unclear cases, a skin biopsy and laboratory tests may be recommended.
8. Can Ayurveda help manage psoriasis naturally?
Ayurveda focuses on balancing internal factors through diet, lifestyle changes, herbal medicines, and external oil applications to support long-term skin health.
9. How long does Ayurvedic psoriasis treatment take to show improvement?
Improvement timelines vary depending on severity, duration of the condition, and consistency with treatment, diet, and lifestyle guidance.
10. Is psoriasis completely curable?
Psoriasis is a chronic condition. While it may not have a permanent cure, proper management can help control symptoms, reduce flare-ups, and improve quality of life.